 In the old days, the only treatment for a painful or infected tooth was to extract it. Over the last several decades, endodontic, or root canal therapy has been developed into a highly reliable method of salvaging such teeth for a long, comfortable, functional life. It is a complex subject, though, and there are potential complications that need to be discussed.
In the old days, the only treatment for a painful or infected tooth was to extract it. Over the last several decades, endodontic, or root canal therapy has been developed into a highly reliable method of salvaging such teeth for a long, comfortable, functional life. It is a complex subject, though, and there are potential complications that need to be discussed.
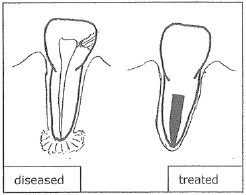
The “root canal” of a tooth is the space deep inside where the nerve, or pulp, is normally found in a healthy tooth. Pain, hypersensitivity, or infection of the pulp can be caused by trauma, or by tooth decay bacteria that have penetrated deep into the tooth. Treatment involves cleaning the inflamed or infected material out of the root canal, and filling it, to seal it up. The body can then usually heal any infection that had spread beyond the tooth, into the surrounding jawbone. Antibiotics are often required to make the treatment successful and ensure that a patient can get numb during the procedure.
We are frequently asked why an infected tooth can’t be cured by a course of antibiotics alone, without doing the formal root canal treatment. The answer is that once the inner root canal space of a tooth is infected, the pulp tissue and its blood supply are destroyed. The white blood cells, which normally fight infection, can no longer get into the tooth. The root canal space then only contains infected debris, which continually seeds bacteria out into the surrounding jawbone, as if it were an infected splinter. The infection will never fully go away until the root is cleaned out and sealed.
Pain can be a factor in root canal therapy. The worst pain usually comes from the problem that leads to the need for treatment in the first place and the treatment just makes it better. Pain following treatment is unpredictable, ranging from no pain at all, to pretty darn sore for a few days. You are welcome to stronger prescription pain medicine, if needed.
After the treatment. A root canal treated tooth is more brittle than it was before treatment, and it is often advisable to put a crown on such a tooth to keep it from breaking. Please note – the restoration of the outside of the tooth, whether it needs a crown or a filling, is a separate procedure, with a separate fee.
Complications. Root canal therapy has a 90 – 95% long-term success rate. This implies that roughly 5 – 10% of cases will experience persistent pain or infection, and require further treatment. There are many things which can compromise the result, including:
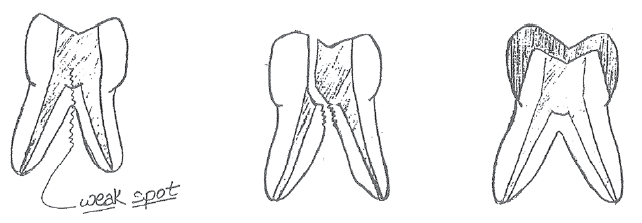
- Fractured root
- Microscopic side canals which can’t be cleaned adequately
- Particularly resistant bacteria in the infection
- A broken instrument lodged in the root canal (a rare occurrence)
- Mystery factors, problems we can never account for
Further treatment can mean repeating the process of cleaning and filling the root, or it can involve surgery to treat the ends of the roots directly. On rare occasions, all goes wrong, and the tooth must be extracted.
Standard and alternative methods.
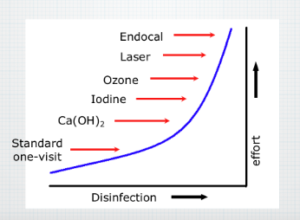
The standard method of filling root canals, which prevails in the United States, is based on the theory that it is most important to disinfect and seal up the root canal, to prevent leakage. Bacteria that cause infections are thereby denied sanctuary inside the canal. Such a root filling is like a cork, composed of gutta percha, a form of rubber, and dental cements. This technique has an excellent record of getting rid of pain and overt infection.
However, there is more to the root of a tooth than the main channel of the root canal, and the alternative method of filling root canals is based upon this anatomical fact. The whole structure of the tooth is actually porous, shot through with microscopic tubules. The bacteria that cause the tooth to be infected may also get into these microscopic spaces, and are not affected by a gutta-percha filling that is only placed in the main canal without first disinfecting with calcium hydroxide. They can remain alive in the porous structure of the tooth, excreting waste products that can add to immune and toxic stress in susceptible people.
The alternative method of filling root canals is an attempt to treat this latent infection of the porous structure with additional disinfection procedures, using a laser and ozone, and by filling the root with calcium oxide prior to a permanent root seal. The calcium hydroxide diffuses through the microscopic tubules, making the environment too alkaline for the bacteria to tolerate. The idea that this method disinfects the root more thoroughly. This type of treatment has the same long term rate of success as the standard gutta percha technique.
In our office, we favor the alternative method of treating root canals, because of the opportunity for enhanced disinfection of the root. It takes one or more additional appointments than the standard method. If you would rather have the more standard root filling, we will be happy to refer you to a specialist for that type of treatment.
We often recommend a crown after root canal treatment. A tooth that needs root canal treatment usually starts off with a big filling or cavity, which means that it is already weakened. In the process of doing the treatment we drill out the rest of the center of the tooth to gain access to the canal, thereby weakening it further. After the root is treated the tooth may become more brittle. All of this adds up to an increased danger that the tooth will break under normal chewing forces. Most teeth that break this way cannot be fixed, and must be extracted. Therefore, we usually recommend that a root–treated tooth be fitted with a crown, which can hold it together and dramatically reduce the chances of the tooth breaking.