Periodontal Disease – Gum Disease
1. What is it?
Gum conditions are quite prevalent, although most people affected have the milder, non-destructive irritations of gingivitis. Gums can be red, swollen, and bleed easily, but without structural damage. Gingivitis clears up readily with routine in-office cleaning and good home hygiene habits.
What we’re really concerned with is the less frequent, but more serious periodontitis, which features damage to the structures that hold teeth in the jawbone.
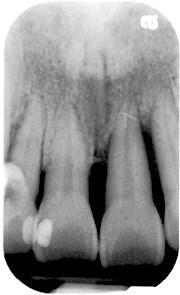
Consider the teeth in this x-ray. The tooth on the left is wrapped with jawbone, holding it firmly in place.
The tooth on the right only has bone holding the tip of the root. The missing bone tissue was destroyed by the action of periodontal disease.
This condition often develops completely without symptoms, but eventually the tooth becomes loose, drifts out of position, and ultimately falls out. Sometimes in the late stages, an overt infection sets in, with pain and swelling.
This disease process causes the majority of tooth loss in adults. Its signs usually emerge in early middle age, though sometimes in younger individuals. It is one of the main things we look for in every dental examination, and if it’s present we always hope to find it in the earliest stages.
2. What causes it?
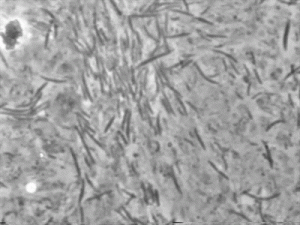
Periodontal disease is caused by uncontrolled masses of bacteria.
Periodontal disease is caused by an unfortunate combination of specific, particularly irritating bacteria, and the body’s reaction to them. The destruction it causes is, very literally, collateral damage in the war between the germs and the white blood cells.
Of the hundreds of bacterial species that occur in the human mouth, only a few are considered to be the main pathogens of gum disease. They are not rare, but not everyone harbors them. Likewise, it takes a strong, even an exaggerated, immune response to those pathogens to create the conditions for destructive periodontal disease.
3. How do we detect it?
The most frequent, reliable method is the basic clinical exam and x-rays, in which we probe the gums for any early signs of damage. We look for “pockets” in the gums, probing around each tooth, and evidence of bone loss on the x-rays.
4. What can we do about it?
Treatment options for periodontal disease range from the toothbrush to surgery. In our biologically oriented practice, we try to create conditions that arrest the disease process. It boils down to two strategies:
- Reducing the bacterial load, by cleaning teeth and killing the germs;
- Making sure the body is well enough nourished to support the continual healing that must take place in the gum tissues.
5. Cleaning teeth and killing germs:
People who have real gum disease cannot afford to be casual about cleaning their teeth. Control of the disease requires thorough professional cleaning to start, attention to home care every day, and professional cleaning three or four times a year. It’s a matter of perpetual maintenance, because the germs will always grow back.
We will coach our patients on the best methods to use at home to keep the teeth clean.
[spoiler title=”Click for: Tricks for cleaning your teeth”]
-
- Do you really know how to brush your teeth? Not everyone does. First of all, don’t aim the brush at the tooth, aim instead for the gum line, where all the action takes place. Angle the brush up into the gums for upper teeth, down for lower teeth.
- Don’t saw away with the brush, that can be very abrasive. Gentle pressure, jiggling, circular motion for a few seconds, pick up the brush and go to the next spot.
- Don’t miss the back sides of the teeth. Every surface needs to be brushed.
- A sonic brush can be very helpful, because the motor does the jiggling work for you.
- Dry brushing – if you have gum disease, you can help yourself by spending a lot of idle time working the brush into the gums. The point of dry brushing is to break up the biofilm of germs, and to mix air into the gums. Most of the bad bacteria are anaerobic, and don’t tolerate oxygen. The more air they are exposed to, the less they like it.
- Floss and/or interdental brushes – gotta do it, there’s as much area between the teeth as on the sides.
- Pocket irrigation – If you do have deeper pockets in the gums, it’s much harder to clean them effectively. A brush and floss will only reach about a millimeter into the crevice. To get under the gums more thoroughly we will have to teach you to use an irrigator, with either a hand syringe, or a pump, like a Water Pik, or Via-Jet. This technique involves flushing under the gums with a disinfecting solution. You can use:
- Salt water
- Diluted hydrogen peroxide (half-half water)
- Salt water with a few drops of iodine (Betadine)
- Water with a few drops of bleach
- Water with ozone bubbled through it from an ozone generator
- A variety of herbal formulas
[/spoiler]
6. Nutrition in periodontal disease:
Breakdown of periodontal tissues indicates that the destructive process has overcome the body’s ability to resist and heal. Resistance and healing depend on the cells having the resources to repair and regenerate. That means nutrition!
A good diet, plenty of vitamins, minerals, protein, essential fats, etc., a minimum of processed foods and sugars – it’s all good advice. It’s worth the trouble to consult with a nutrition professional to identify elements you may be deficient in, to identify foods you don’t tolerate, and to be sure your diet is most appropriate for you.
Beyond good basics, there are a few specific nutrients that are most commonly deficient in gum disease, and should be supplemented.
[spoiler title=”Click for: specific nutrients for periodontal disease”]
-
- Vitamin C – required for making collagen, therefore essential for any connective tissue healing. Symptoms of scurvy, the fatal deficiency of vitamin C include the teeth loosening and falling out, so we can consider gum disease a form of localized scurvy. To find out how much vitamin C you really need, see this website for advice.
New on the horizon is the “liposomal” form of vitamin C, which delivers directly into cells. Lower doses are used with this form. - Vitamin D – required for absorption of calcium, and lots of other necessary things, so essential for bone healing and maintenance. There is a common blood test for vitamin D levels. Most nutritional doctors recommend you maintain 50-80 nanograms per ml. That is a lot of sunshine, or take supplements.
- Coenzyme Q-10 – This is a quasi-vitamin, because your body can make it on its own, but tissues that are aging or unwell tend to be deficient, and taking it as a supplement can replenish deficient tissues. CoQ10 is the keystone in the brick oven of cellular energy production (the mitochondria). When it’s deficient, the oven smokes (makes free radicals) and doesn’t provide the cells with enough energy. With enough CoQ10, tissues can heal, and white blood cells are more effective.
- Trace Minerals – Some elements are toxic, like mercury and arsenic, while others are essential to heath, like vanadium and chromium. Do you know if you get enough boron in your diet, or selenium? We recommend our Zing liquid trace mineral formula, for all the obscure cofactors that are required for healing.
- Vitamin C – required for making collagen, therefore essential for any connective tissue healing. Symptoms of scurvy, the fatal deficiency of vitamin C include the teeth loosening and falling out, so we can consider gum disease a form of localized scurvy. To find out how much vitamin C you really need, see this website for advice.
[/spoiler]
